In today’s fast-paced lifestyle, managing blood sugar levels has become a growing concern not just for individuals with diabetes, but for anyone aiming to maintain steady energy, better metabolism, and long-term health. One of the most effective yet often overlooked nutritional tools for stabilizing blood sugar is dietary fiber.
At SmartBite Nutrition , we believe that smarter eating starts with understanding how food works in your body. Let’s explore how fiber plays a crucial role in preventing sudden spikes in blood sugar and why it deserves a central place in your daily diet.
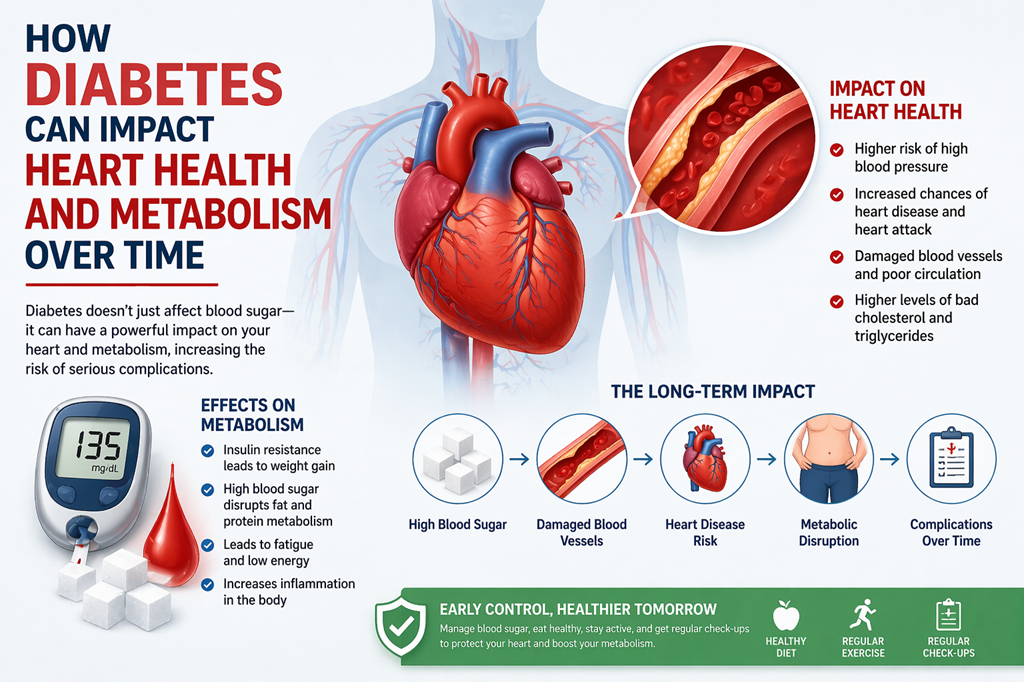
What Happens During a Blood Sugar Spike?
When you consume carbohydrate-rich foods especially refined ones like white bread, sugary snacks, or processed meals your body quickly breaks them down into glucose. This leads to a rapid rise in blood sugar levels, often followed by a sharp drop. These fluctuations can cause fatigue, cravings, irritability, and over time, increase the risk of insulin resistance and metabolic disorders.
How Fiber Helps Stabilize Blood Sugar
Fiber, particularly soluble fiber, acts as a natural regulator in this process. Unlike simple carbohydrates, fiber is not digested quickly. Instead, it slows down the absorption of sugar into the bloodstream, leading to a more gradual and controlled rise in blood glucose levels.
Here’s how fiber works its magic:
- Slows Digestion
Fiber forms a gel-like substance in the gut, which delays the breakdown of carbohydrates. This means glucose enters the bloodstream more slowly, preventing sudden spikes. - Improves Insulin Sensitivity
A fiber-rich diet helps your body use insulin more effectively, allowing cells to absorb glucose efficiently and maintain balanced blood sugar levels. - Promotes Satiety
High-fiber foods keep you fuller for longer, reducing the likelihood of overeating or reaching for sugary snacks that can trigger glucose surges. - Supports Gut Health
Fiber feeds beneficial gut bacteria, which play a role in metabolic health and can indirectly influence blood sugar regulation.
Types of Fiber That Matter
Not all fiber is created equal. To manage blood sugar effectively, it’s important to include both:
- Soluble Fiber: Found in oats, legumes, fruits like apples and berries, and seeds like chia and flax. This type directly helps in slowing glucose absorption.
- Insoluble Fiber: Found in whole grains, vegetables, and nuts. While it doesn’t directly impact blood sugar, it supports digestion and overall gut health.
A balanced intake of both types ensures comprehensive benefits.
Simple Ways to Add More Fiber to Your Diet
Incorporating fiber doesn’t require a complete diet overhaul. Small, consistent changes can make a big difference:
- Start your day with oatmeal topped with fruits and nuts
- Choose whole fruits instead of juices
- Replace refined grains with whole grains like brown rice or millets
- Add a portion of legumes such as lentils or chickpeas to your meals
- Include a side of vegetables in every meal
Smart Eating with SmartBite
At SmartBite Nutrition , we design meals that are not only delicious but also thoughtfully balanced to support your health goals. Our approach emphasizes whole ingredients, optimal fiber content, and low glycemic impact. helping you stay energized and in control throughout the day.
Fiber is more than just a digestive aid, it’s a powerful ally in managing blood sugar levels. By slowing down glucose absorption, improving satiety, and supporting metabolic health, fiber helps you avoid the highs and lows that come with blood sugar spikes.
Making fiber-rich foods a regular part of your diet is a simple yet impactful step toward better health. With SmartBite, eating smart becomes effortless and your body will thank you for it.
Start small, stay consistent, and let fiber do the heavy lifting.